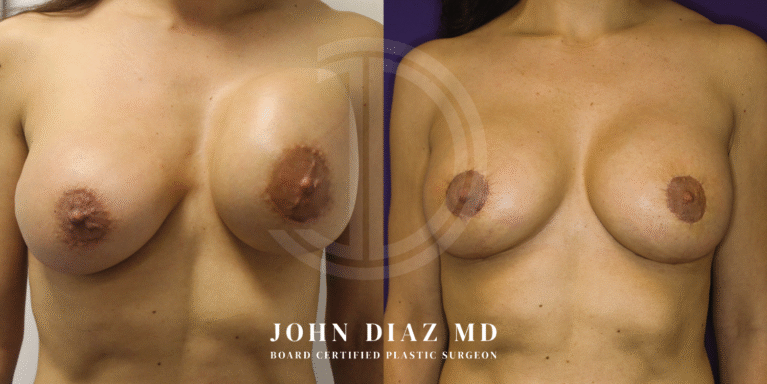
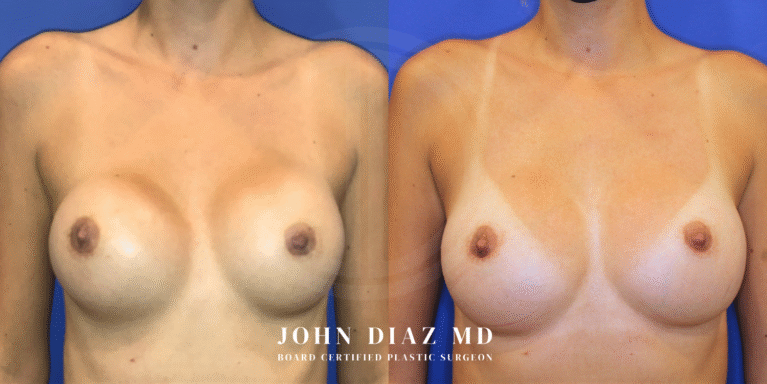
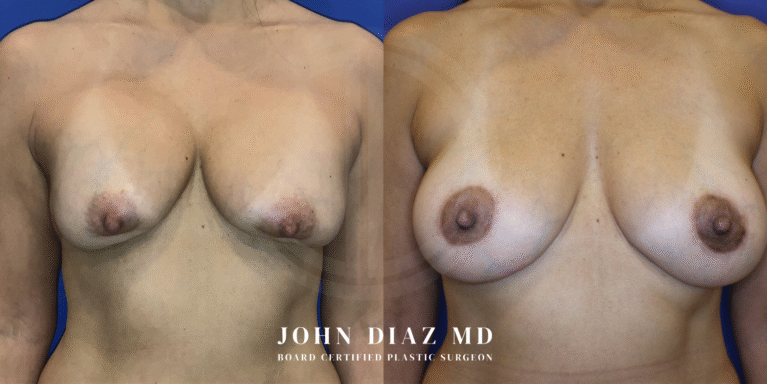
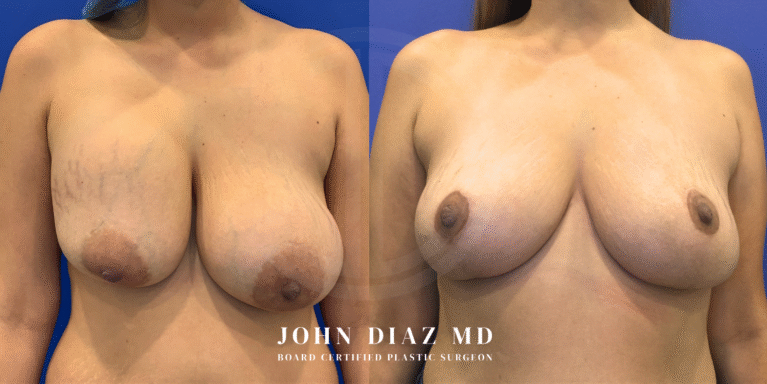
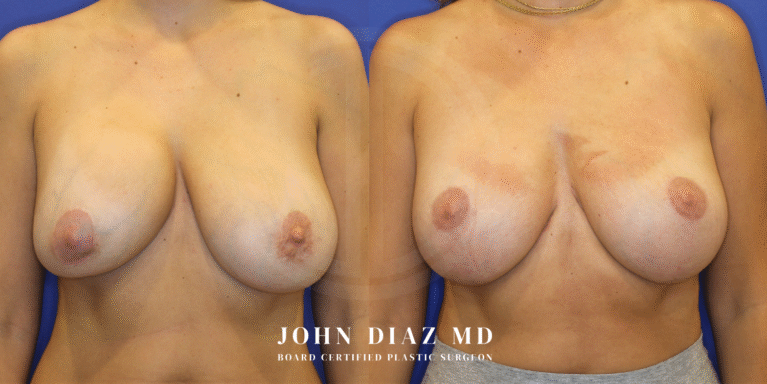
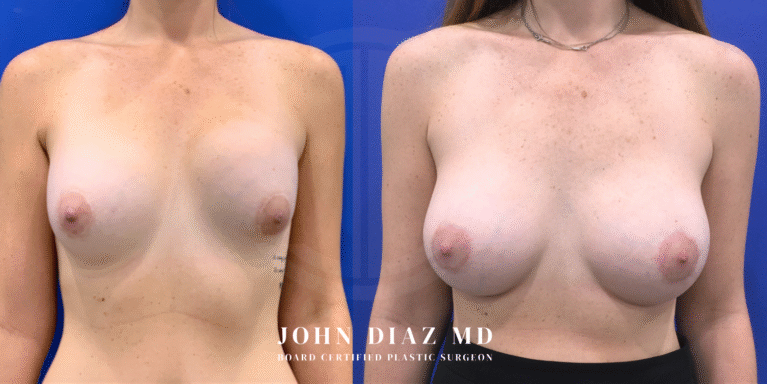
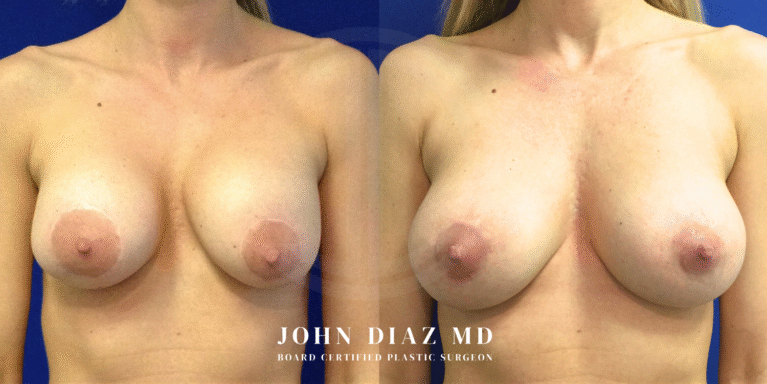
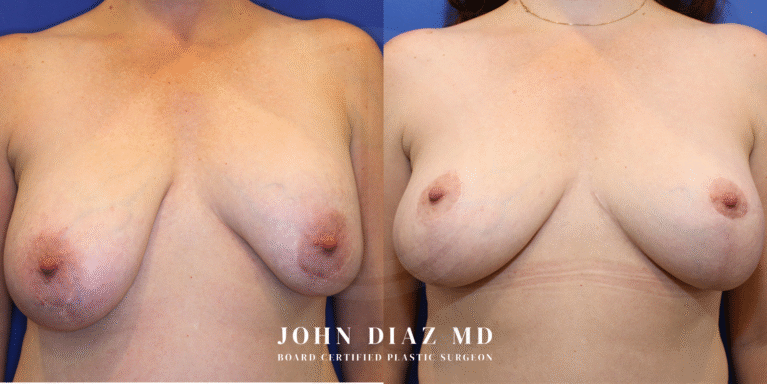
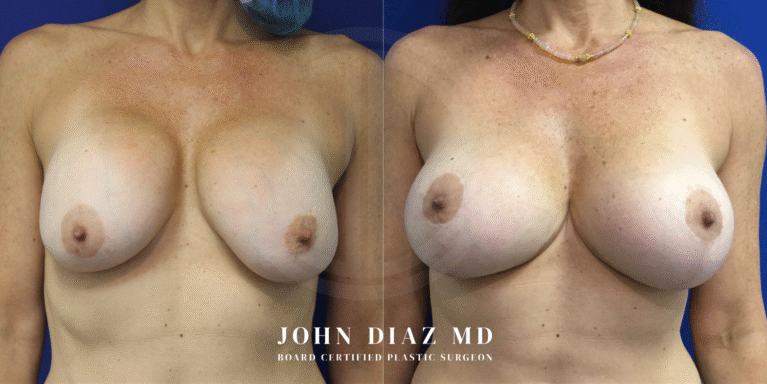
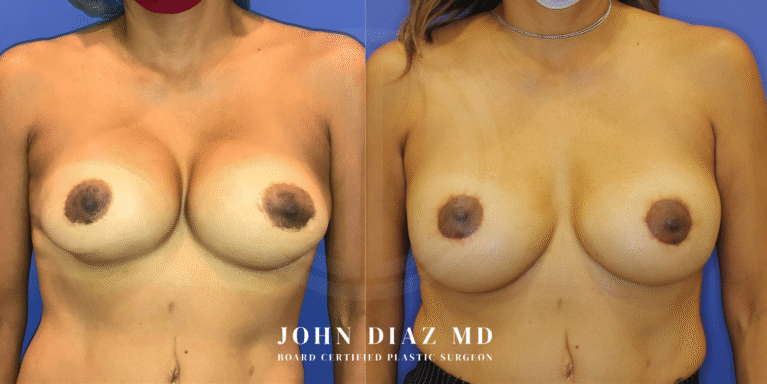
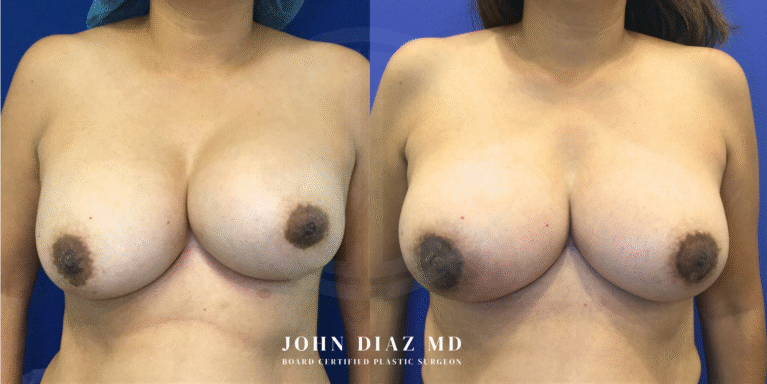
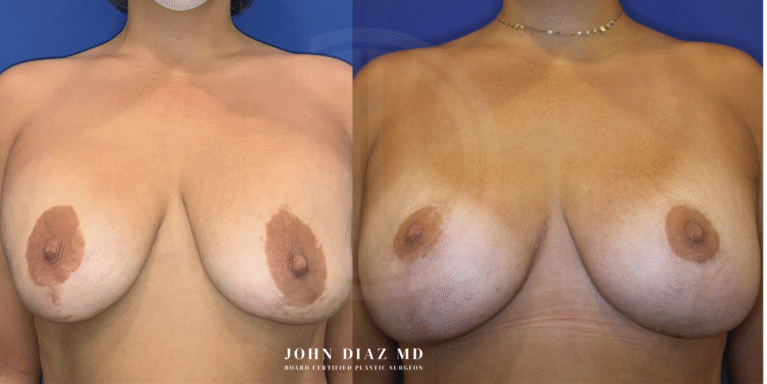
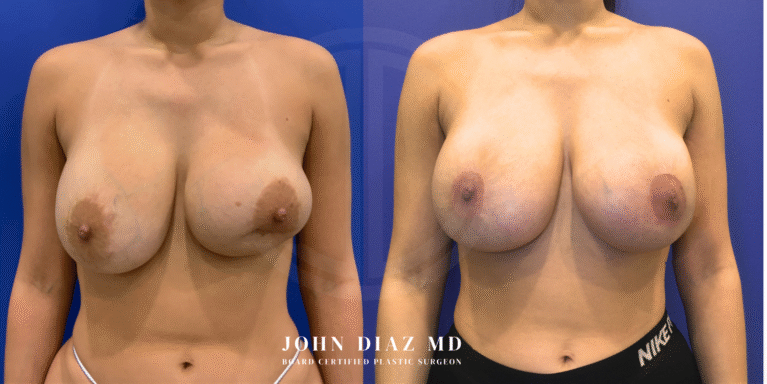
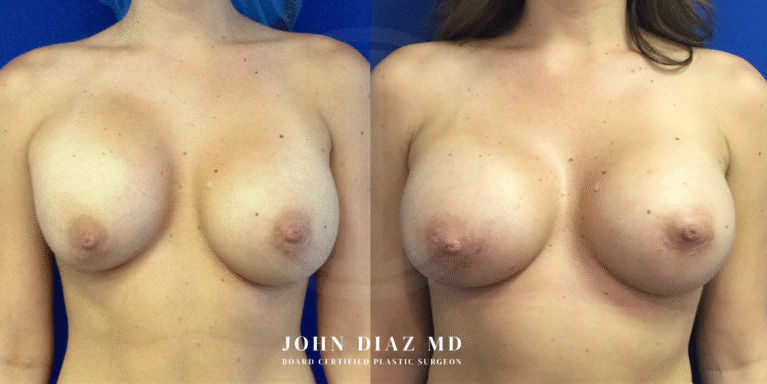
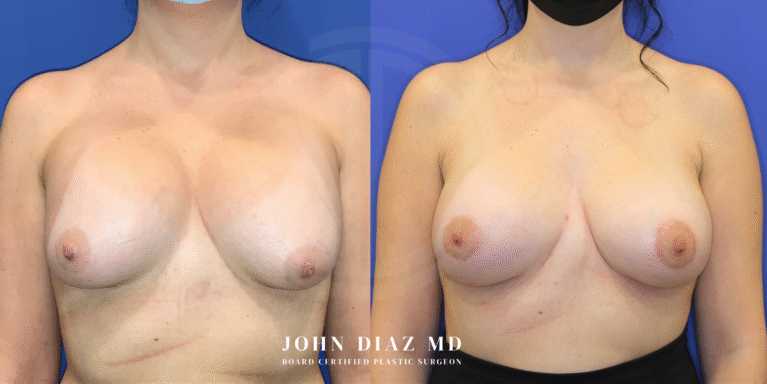
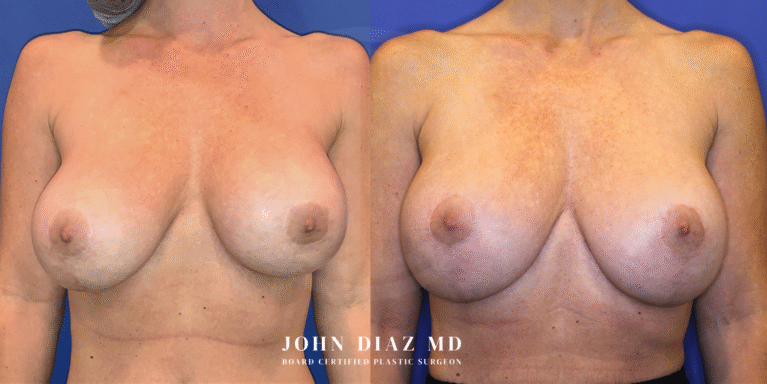
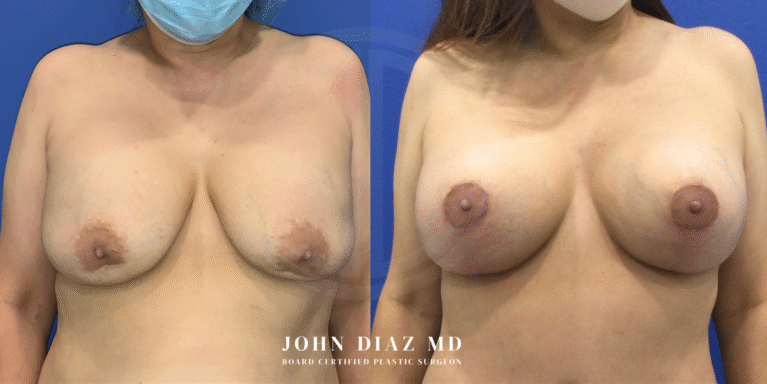
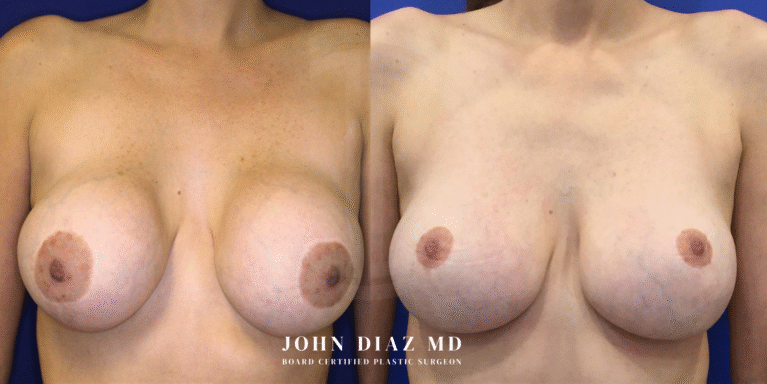
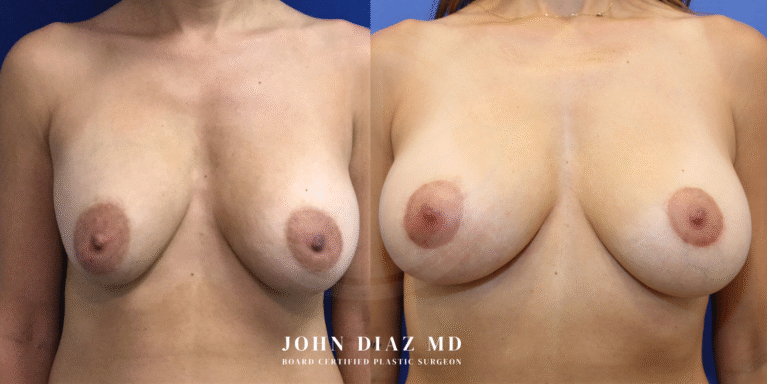
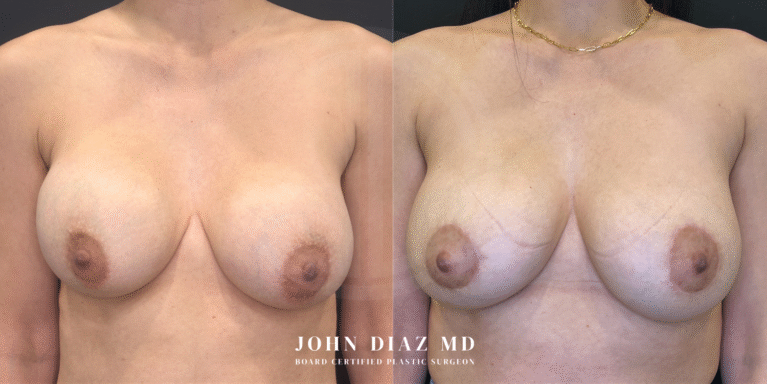
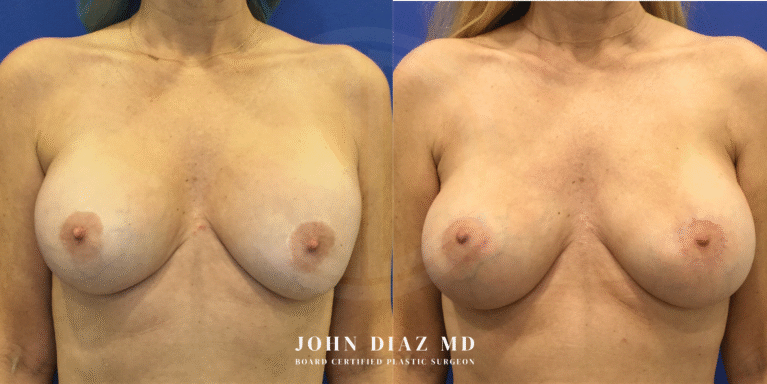
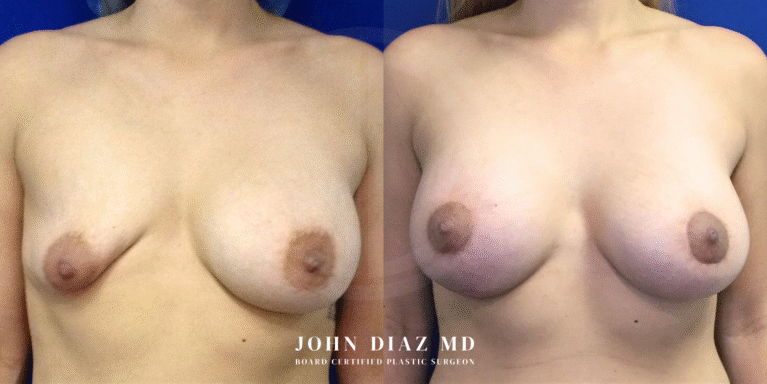
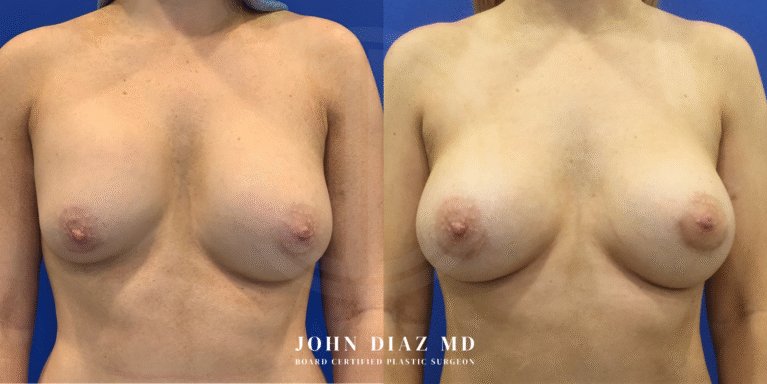
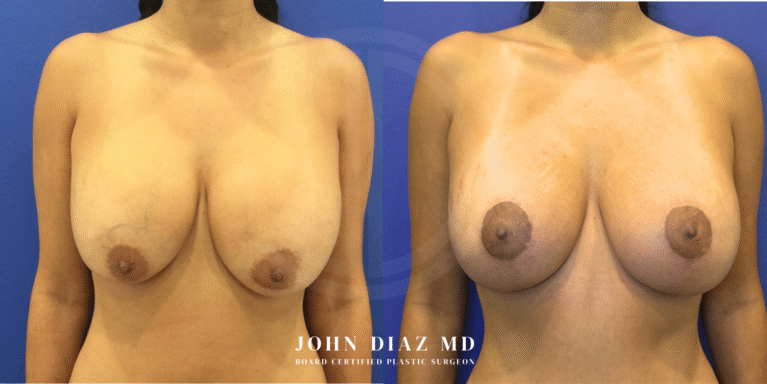
What to Expect During Your Breast Revision Experience
Speak with Our Surgical Coordinator
Curious about breast revision surgery? Begin your journey with a one-on-one consultation with our Surgical Coordinator from the comfort of your home. During this initial conversation, you’ll discuss your goals, review details about cost, scheduling, recovery, and payment options, and have all your questions answered. This informative, no-obligation discussion is designed to help you make a confident and informed decision about your next step.
Consultation & Discussion with Dr. John Diaz
During your full-hour consultation, Dr. Diaz will carefully review your previous surgical results and listen to your concerns. We’ll discuss your goals in detail and explain your options for revision, whether they involve implant removal, replacement, or lift techniques.
Physical Examination
Dr. Diaz performs a thorough evaluation of your current breast condition, including implant position, scar tissue formation, and tissue quality. This comprehensive assessment helps determine the optimal revision approach.
3D Simulation & Surgical plans
Every revision is different. Dr. Diaz will design a personalized plan based on your anatomy, surgical history, and goals. Using VECTRA 3D imaging, Dr. Diaz creates a computer simulation of your breasts after the breast revision surgery. He will review the recommended techniques, incision placements, and expected outcomes in clear, honest language.